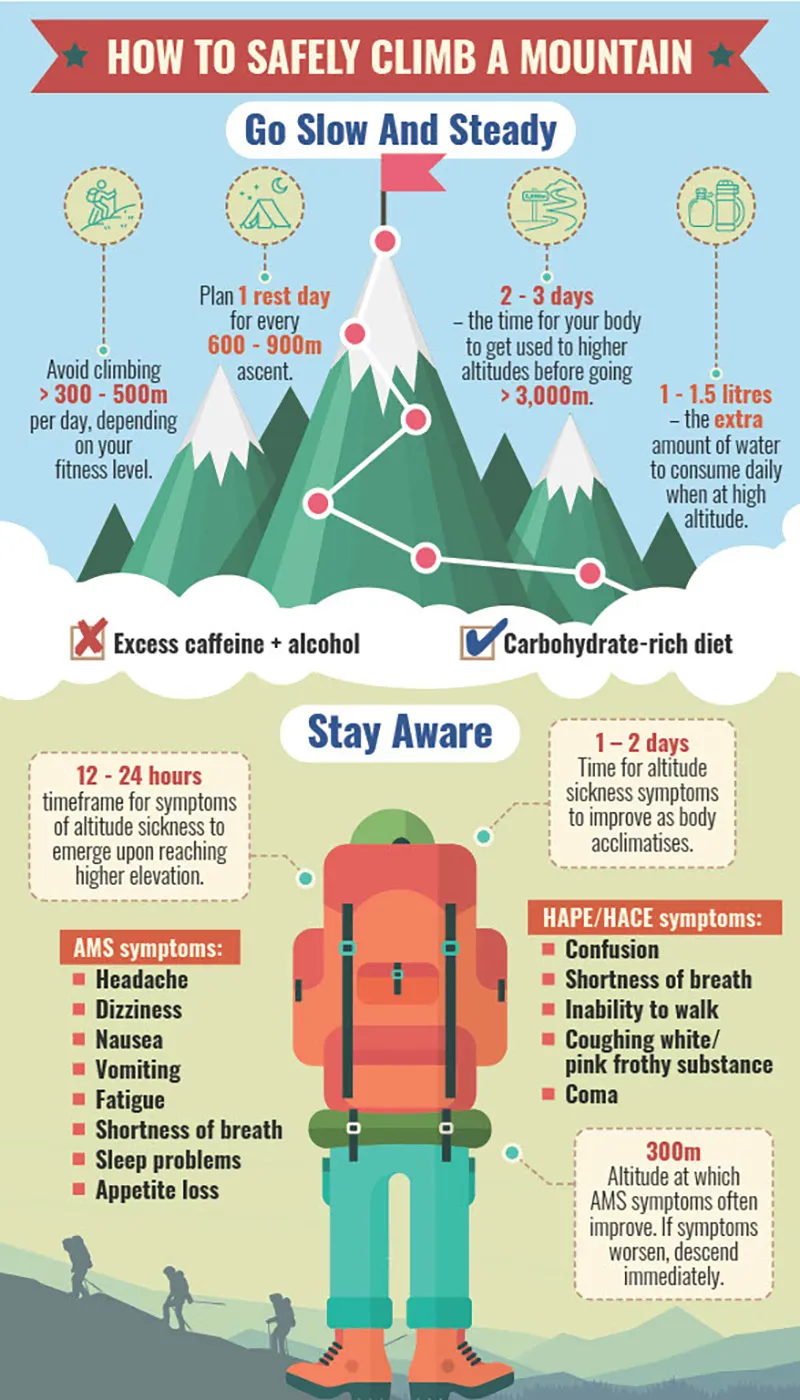
Complete Guide to Altitude Sickness Prevention: Essential Tips for High-Altitude Travel
During my years of guiding climbers through the Rocky Mountains and the Andes, I've witnessed firsthand how proper altitude sickness prevention can make the difference between a successful summit and a dangerous evacuation. This comprehensive guide combines medical expertise with practical field experience to help you safely enjoy high-altitude adventures. Whether you're planning a trek to Everest Base Camp or a ski trip to Colorado, understanding how to prevent altitude sickness is crucial for your safety and enjoyment. Nature Guests has compiled the most effective strategies used by professional mountain guides worldwide.
Understanding Altitude Sickness
Altitude sickness, medically known as acute mountain sickness (AMS), occurs when your body cannot adjust quickly enough to the decreased oxygen levels at high elevations. Having guided expeditions across various mountain ranges, I've observed that effective altitude sickness prevention begins with understanding the physiological changes that occur as we ascend.
At sea level, the atmospheric pressure allows our lungs to absorb oxygen efficiently. However, as elevation increases, air pressure decreases exponentially. At 10,000 feet, there's approximately 30% less oxygen than at sea level. Your body responds by increasing breathing rate, heart rate, and eventually producing more red blood cells – a process called acclimatization.
The three main types of altitude illness include Acute Mountain Sickness (AMS), High Altitude Pulmonary Edema (HAPE), and High Altitude Cerebral Edema (HACE). AMS is the most common, typically manifesting as headaches, nausea, fatigue, and sleep disturbances. During my expeditions in the Himalayas, I've seen that travelers who understand these mechanisms are better equipped to implement proper altitude sickness prevention strategies.

Risk Factors and Individual Susceptibility
Physical fitness doesn't prevent altitude sickness – I've seen Olympic athletes struggle while less fit individuals adapt quickly. Age, genetics, and previous exposure to altitude play more significant roles. Interestingly, people living at sea level may be more susceptible than those from moderate elevations.
Pre-existing conditions like heart disease, lung problems, or sleep apnea increase risk. If you have chronic conditions, consult a physician familiar with high-altitude medicine before planning your trip. This is especially important for emergency preparedness in remote mountain areas.
Gradual Ascent Strategies
The cornerstone of effective altitude sickness prevention is controlled ascent. After leading over 200 high-altitude expeditions, I can confidently say that rushing altitude gain is the most common mistake I see climbers make. The key principle is simple: "climb high, sleep low."
The Golden Rules of Ascent
- Below 8,000 feet: Ascend at any comfortable rate
- 8,000-9,000 feet: Sleep at this elevation for 1-2 nights before going higher
- Above 9,000 feet: Increase sleeping elevation by no more than 1,500 feet per day
- Every 3,000 feet: Include an extra rest day for acclimatization
During my time guiding in the Colorado Rockies, I've refined this approach based on real-world conditions. Weather windows, group dynamics, and logistical constraints sometimes require flexibility, but these principles remain the foundation of safe ascent planning.
Effective Strategies
- Plan rest days into your itinerary
- Use staging camps for gradual ascent
- Consider pre-acclimatization training
- Monitor team members' condition daily
Common Mistakes
- Flying directly to high-altitude destinations
- Ignoring early symptoms to maintain schedule
- Ascending with altitude sickness symptoms
- Underestimating individual variation
Professional mountaineering expeditions often use "acclimatization rotations" – repeated cycles of ascending to higher camps and returning to lower elevations. This strategy, while time-consuming, significantly improves success rates and safety margins. For recreational climbers, modified versions can be equally effective for altitude sickness prevention.
Essential Medications and Supplements
Pharmacological altitude sickness prevention can be highly effective when used appropriately. During expeditions to peaks above 14,000 feet, I always carry a comprehensive medical kit including altitude-specific medications. However, these should complement, not replace, proper acclimatization techniques.
Acetazolamide (Diamox)
The gold standard for altitude sickness prevention, acetazolamide works by inhibiting carbonic anhydrase, which stimulates breathing and speeds acclimatization. I recommend starting 125mg twice daily, beginning 24 hours before ascent.
Side effects include tingling in fingers and altered taste of carbonated beverages. Despite being a sulfonamide, allergic reactions are rare. Based on my experience guiding hundreds of climbers, the benefits far outweigh the minor side effects for most people.
Alternative Medications
Dexamethasone: A steroid that can prevent and treat severe altitude sickness. I reserve this for emergency situations or when acetazolamide is contraindicated. The standard dose is 2mg every 6 hours.
Ibuprofen: Recent studies show 600mg three times daily can prevent altitude headaches. It's particularly useful for climbers who prefer over-the-counter options or have contraindications to prescription medications.
Natural Supplements: While evidence is limited, some climbers report benefits from ginkgo biloba, iron supplements (for those with deficiency), and antioxidant complexes. These should be considered supplementary to proven methods.
Important Medical Considerations
Always consult with a physician familiar with altitude medicine before taking any medications. Some climbers develop overconfidence with medication and ignore proper acclimatization practices. Remember, no medication can substitute for gradual ascent and proper wilderness safety protocols.
Carry a comprehensive first aid kit and ensure at least one team member has wilderness first aid training. Altitude emergencies can escalate rapidly, and proper preparation saves lives.
Hydration, Nutrition, and Lifestyle Factors
Proper hydration and nutrition form critical components of altitude sickness prevention. At altitude, your body loses water more rapidly through increased respiration and lower humidity. I've observed that dehydration often mimics or exacerbates altitude sickness symptoms, making proper fluid intake essential.
Hydration Strategies
Aim for 3-4 liters of fluid daily at altitude, but avoid overhydration which can lead to hyponatremia. I teach climbers to monitor urine color – pale yellow indicates proper hydration. Clear urine suggests overhydration, while dark yellow indicates dehydration.
Electrolyte balance becomes crucial at altitude. I recommend carrying electrolyte supplements or tablets, particularly for multi-day expeditions. Avoid excessive caffeine and alcohol during the first 48 hours at altitude, as they can interfere with acclimatization and worsen dehydration.
Nutritional Considerations
At altitude, your body requires 10-15% more calories due to increased metabolic demands. Focus on carbohydrate-rich foods, which are more efficiently metabolized in low-oxygen environments. I've found that climbers who maintain steady blood sugar levels experience fewer altitude sickness symptoms.
Iron-rich foods support oxygen transport, though iron supplements should only be taken if deficiency is diagnosed. Avoid large meals that can divert blood flow from acclimatization processes. Instead, eat smaller, frequent meals throughout the day.
Expert advice on high-altitude travel preparation
Sleep and Recovery
Quality sleep is often compromised at altitude due to periodic breathing patterns. This is normal but can be minimized through proper altitude sickness prevention techniques. Sleep medications should be avoided as they can depress breathing.
I encourage climbers to practice good sleep hygiene: maintain regular sleep schedules, keep sleeping areas well-ventilated, and avoid late-evening strenuous activity. If sleep quality remains poor after 3-4 nights, consider descending to a lower elevation.
Temperature regulation becomes more challenging at altitude. Layer clothing systems allow for fine-tuning body temperature, which affects sleep quality and overall comfort. Poor sleep can significantly increase susceptibility to altitude sickness.
Recognizing and Responding to Symptoms
Early recognition of altitude sickness symptoms is crucial for effective altitude sickness prevention and treatment. During my guiding career, I've developed systematic approaches for monitoring team health that have prevented numerous emergency evacuations.
Mild Altitude Sickness (AMS) Symptoms
- Headache (often the first symptom)
- Nausea and loss of appetite
- Fatigue and weakness
- Dizziness and lightheadedness
- Sleep disturbances
- General malaise ("feeling unwell")
Severe Symptoms Requiring Immediate Action
- HACE signs: Confusion, loss of coordination, altered mental status
- HAPE signs: Severe shortness of breath, cough with frothy sputum
- Inability to walk in a straight line
- Severe headache unresponsive to pain medication
- Vomiting preventing fluid intake
I use daily symptom checks with team members, rating headache, nausea, fatigue, and dizziness on a 1-10 scale. Trends are more important than absolute numbers – increasing scores over consecutive days warrant attention even if symptoms seem mild.
Response Protocols
Mild Symptoms:
- Stop ascending and rest at current elevation
- Increase fluid intake and maintain nutrition
- Take pain relief for headaches
- Monitor symptoms every few hours
Severe Symptoms:
- Immediate descent of 1,000+ feet
- Administer oxygen if available
- Consider emergency medications
- Prepare for evacuation if necessary
Remember that altitude sickness can worsen rapidly. When in doubt, descend. I always tell my teams: "It's better to be disappointed at base camp than to become a rescue statistic." If you find yourself in a emergency situation, knowing how to signal for help can be lifesaving.
Essential Gear and Equipment
Proper equipment plays a vital role in altitude sickness prevention and emergency response. After years of testing gear in extreme conditions, I've compiled this list of essential items that can significantly improve your safety and comfort at altitude.
Monitoring Equipment
Pulse Oximeter: Essential for monitoring oxygen saturation levels. I recommend models that work reliably in cold conditions and have good battery life. Normal readings at altitude are lower than sea level – 88-92% is acceptable above 10,000 feet.
Thermometer: Hypothermia risk increases at altitude, and fever can indicate complications. Digital thermometers work best in cold conditions with proper battery management.
Oxygen Support
Portable Oxygen Concentrator: For serious expeditions or individuals with pre-existing conditions, portable oxygen can be lifesaving. Modern units are remarkably compact and efficient.
Emergency Oxygen: Compressed oxygen canisters provide temporary relief but have limited capacity. Reserve these for emergency situations or short-term symptom relief.
Training and Preparation Equipment
Pre-acclimatization training can significantly improve your body's response to altitude. While living at sea level, several tools can help simulate altitude conditions and improve your physiological preparation.
Altitude Training Masks: While controversial, some athletes report benefits from training masks that restrict airflow. These don't truly simulate altitude but can improve respiratory muscle strength and breathing efficiency.
Hypoxic Training Systems: More sophisticated systems can create low-oxygen environments for sleep or exercise. Professional mountaineers sometimes use these for specific expedition preparation, though they require significant investment.
The most effective preparation remains consistent cardiovascular training and, when possible, spending time at moderate altitudes (6,000-8,000 feet) before attempting higher elevations. This is particularly important if you're planning routes where navigation skills become critical.
Emergency and Communication Gear
Satellite Communication: In remote areas, satellite communicators or PLBs (Personal Locator Beacons) can summon rescue when altitude emergencies occur. I consider these essential for expeditions beyond cell coverage.
First Aid Supplies: Include altitude-specific medications, thermometer, and items for treating hypothermia. Consider taking a wilderness first aid course before departure.
Weather Protection: Altitude amplifies weather risks. Quality insulation, waterproof layers, and backup systems become critical when altitude sickness impairs judgment or mobility.
Navigation Tools: GPS units, maps, and compass skills become vital when altitude affects mental clarity. Redundant navigation systems prevent dangerous mistakes in challenging conditions.
Conclusion
Effective altitude sickness prevention combines scientific understanding with practical field experience. Throughout my career guiding expeditions across major mountain ranges, I've seen how proper preparation transforms challenging ascents into safe, enjoyable adventures. The strategies outlined in this guide represent decades of collective experience from the mountaineering community.
Remember that altitude affects everyone differently, and what works for one person may not work for another. The key is preparation, vigilance, and the willingness to adjust plans based on conditions. Never let summit fever override safety considerations – mountains will always be there for future attempts.
Start implementing these altitude sickness prevention techniques on smaller peaks before attempting major expeditions. Build experience gradually, learn to recognize your body's responses, and develop the judgment that comes only through practice. Consider this guide a starting point for your high-altitude education, not the final word.
Most importantly, travel with experienced partners, maintain communication with support teams, and always have contingency plans. The mountains teach humility, patience, and respect for natural forces. Embrace these lessons, and your high-altitude adventures will be both safer and more rewarding. For more comprehensive wilderness safety information, visit our complete altitude sickness prevention resource and continue your education in mountain safety.
Ready to Plan Your High-Altitude Adventure?
Equip yourself with the essential gear and knowledge for safe mountain travel. Remember, proper preparation is the foundation of successful high-altitude expeditions.



